Mouth Gut Microbiome Axis: Why Your Gut Won't Heal
Feb 23, 2026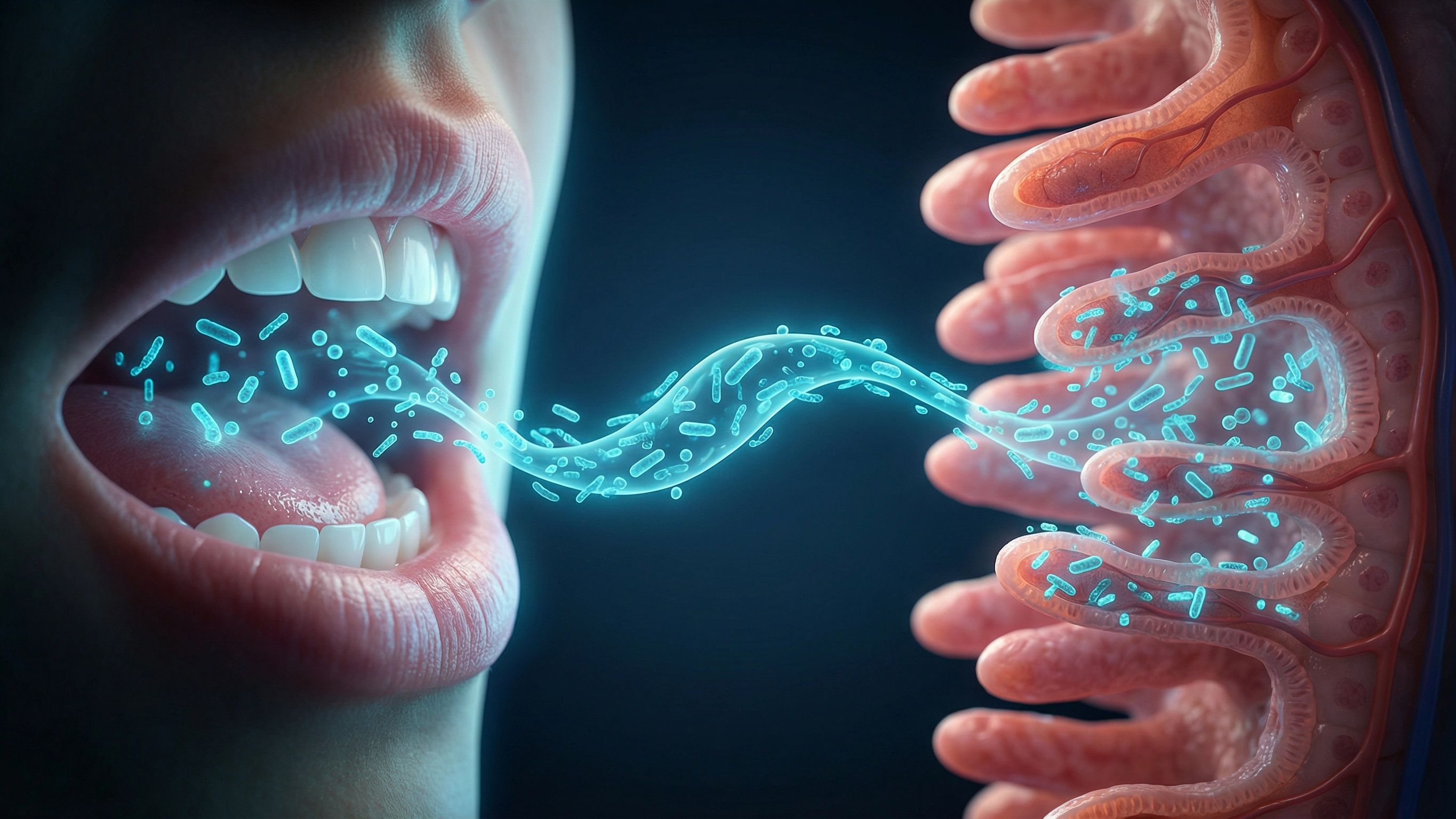
Understanding the mouth gut microbiome axis is the first step to actually healing your gut
I've had this conversation more times than I can count — a patient sitting across from me, frustrated, telling me they've done everything "right."
They've overhauled their diet, taken a rotation of probiotics, cut out gluten, and gone low-FODMAP.
And yet, their digestion is still a mess. Bloating. Unpredictable reactions to food. Persistent inflammation that won't quit.
When I examine their mouth, the picture becomes clearer almost immediately: bleeding gums, pockets of chronic inflammation, an oral microbiome completely out of balance.
The gut has been getting all the attention — and rightfully so. But there's a major piece of the picture that most gut health programs never address: the mouth gut microbiome axis, and the steady, daily migration of oral bacteria directly into your digestive system.
In this article, you'll learn exactly how oral pathogens travel into the gut, which specific bacteria researchers have linked to gut dysbiosis and even colorectal disease, and why healing one system without looking at the other often means starting over from scratch.
Keep reading — what we cover midway through this article may completely reframe how you've been approaching your gut health.
Key Takeaways
- Every day, you swallow roughly 0.75 to 1.5 liters of saliva — loaded with oral bacteria — which seeds your intestinal tract with microbes, for better or worse.¹
- When the oral microbiome is out of balance, swallowed oral pathogens can colonize the gut and drive dysbiosis, especially in individuals whose gut barrier is already compromised.²
- Fusobacterium nucleatum, an oral bacterium, has been consistently identified in colorectal tumor tissue and is considered a significant contributor to gut dysbiosis and colorectal cancer progression.³
- Porphyromonas gingivalis, a primary driver of gum disease, has been shown to alter gut microbiota composition, reduce the expression of gut tight junction proteins, and trigger systemic inflammation when swallowed repeatedly.⁴
- The mouth gut microbiome axis runs bidirectionally — gut dysbiosis can worsen the oral environment, which then feeds more oral pathogens back into the gut in a reinforcing cycle.⁵
- Gut healing protocols that skip the oral microbiome are often treating downstream effects while the upstream source continues unaddressed.
- Comprehensive oral microbiome testing — like the Orobiome package — is one of the most underutilized tools in functional health, and it could be exactly what's been missing from your protocol.
Every swallow is a microbial event
Most people think of their mouth and gut as separate systems.
Anatomically, they're not. They're one continuous tube, and what happens at the top of that tube matters enormously to everything below.
Here's the basic biology: your salivary glands produce between 0.75 and 1.5 liters of saliva daily.¹
That saliva carries a dense load of oral bacteria — some protective, some pathogenic — that travels down the esophagus and into the stomach with every swallow.
Under normal circumstances, stomach acid neutralizes most of these microbes before they can reach the intestines.
But "normal circumstances" is the key phrase.
When someone has chronic gum inflammation, periodontal disease, or a disrupted oral microbiome, the number of pathogenic bacteria being swallowed increases substantially.
And research has shown that during oral dysbiosis, these organisms are far more likely to survive the gastric barrier and colonize the gut — particularly when the intestinal environment is already compromised.²
When both the oral and gut microbiomes are disrupted at the same time, the conditions are essentially set for persistent, treatment-resistant dysbiosis.
This is the oral bacteria and digestive health connection that most health conversations still aren't having.
If you want to go deeper on how oral health shapes chronic disease risk more broadly, this article lays out the research well.
The bacteria you've probably never heard of — and why they matter
Of all the research linking oral bacteria and gut health, two organisms keep appearing in the literature with striking consistency.
The first is Fusobacterium nucleatum (F. nucleatum). This is a gram-negative anaerobe that's a core resident of the human oral microbiome.
In a balanced mouth, it's manageable. The problem arises when it migrates downstream.
Multiple studies — from North American, European, and Asian cohorts — have found F. nucleatum significantly enriched in colorectal tumor tissue compared to healthy colon tissue.³
It reaches the gut through swallowing and through the circulatory system, and once there, it has a remarkable ability to adhere to intestinal tissue and promote inflammation.⁶
A 2021 systematic review published in Cancer Cell International described F. nucleatum as a potential prognostic biomarker for colorectal cancer risk, based on its consistent enrichment in colorectal specimens and its expression of virulence factors that promote tumor progression.³
For people focused purely on gut health, the significance of this is hard to overstate. F. nucleatum is an oral bacterium first. It's an oral microbiome problem that becomes a gut microbiome problem.
The second is Porphyromonas gingivalis (P. gingivalis) — the primary bacterial driver behind gum disease.
When swallowed repeatedly (as happens with ongoing periodontal disease), P. gingivalis has been shown in animal studies to significantly alter gut microbiota composition, reduce expression of gut tight junction proteins in the ileum, raise circulating endotoxin levels, and induce measurable insulin resistance.⁴
In separate research, individuals with periodontal disease were found to have a less diverse intestinal microbiome, with elevated levels of pro-inflammatory taxa that are consistently associated with gut-driven systemic conditions.¹
These findings illustrate exactly how the oral-gut microbiome connection operates in practice — and why treating swallowing oral pathogens as a gut health problem is more than just a metaphor.
Why your gut protocol might keep falling short
Here's where I want to be direct with you, because I see this pattern constantly.
Conventional medicine has done an extraordinary job of advancing what we know about the gut.
Gastroenterologists, internists, and primary care physicians are increasingly aware of the microbiome's role in chronic disease.
The problem isn't a lack of good intention — it's a structural one.
Oral health and systemic medicine have been treated as separate disciplines for nearly two centuries, and that separation means most gut health protocols, even excellent ones, are designed without factoring in the oral microbiome.
So a patient diligently takes probiotics, repairs their gut lining, and improves their diet — genuine, meaningful work.
But if they're also swallowing several hundred milliliters to over a liter of saliva every day that's loaded with P. gingivalis or F. nucleatum, that upstream source of oral bacteria and gut dysbiosis keeps reseeding the problem.
The gut protocol isn't failing because it's wrong. It's failing because it's incomplete.
Research published in Frontiers in Cellular and Infection Microbiology confirmed that oral dysbiosis enhances the likelihood of gut translocation — and that two conditions must exist for oral pathogens to establish themselves in the gut: an elevated load of oral bacteria from dysbiosis, and a disruption to the gut's own resistance mechanisms.⁵
Both systems protect each other. And both can undermine each other when compromised.
This is why we talk so much about the mouth gut microbiome axis at Gateway to Health. It's not a theoretical concept — it has real, practical consequences for anyone who's been chasing gut health without lasting results.
You can also explore the concept of intestinal permeability, and how leaky mouth syndrome relates to the gut problems you may already be familiar with.
The case for dual testing
This is the conversation I wish more functional health practitioners were having: you can't fully understand one microbiome without the other.
Oral microbiome testing — specifically, comprehensive sequencing of the bacterial populations in your mouth — can reveal which pathogens are present at elevated levels before they cause obvious symptoms.
Gum disease isn't always visible or painful in its early stages. Oral dysbiosis can be quietly seeding the gut with problematic bacteria long before you notice bleeding gums or chronic inflammation.
At the same time, gut microbiome testing tells you what's actually happening in the intestinal environment — which species are out of balance, whether the gut barrier is compromised, and how the microbial community is functioning as a whole.
When you test both, the picture becomes dramatically clearer. You're no longer guessing which protocol to follow. You know what you're dealing with and where to start.
And if you want to understand what functional oral health actually looks like as a clinical approach, this article is a good place to start.
What this means practically
The oral-gut microbiome connection is one of the most actionable areas in functional health right now — and one of the least addressed.
If you've been doing the gut health work and still not feeling the way you want to, this is worth exploring seriously.
Start by taking your oral health seriously as a systemic health issue, not just a dental one. Gum inflammation isn't just a gum problem. Bleeding when you floss isn't just "normal."
These are signals that the oral microbiome is out of balance — and that imbalance has a direct pathway into your gut.
And if you're ready to stop guessing and start knowing exactly what's going on, testing both systems together gives you the clearest, most complete picture available.
Your gut may not be healing because your mouth isn't healed yet. That's worth looking into.
Sources
- Can oral bacteria affect the microbiome of the gut?, Journal of Oral Microbiology, 2019.
- Oral pathogens meet the gut microbiome: new mechanistic insights on systemic disease, Frontiers in Cellular and Infection Microbiology, 2025.
- The dysbiosis signature of Fusobacterium nucleatum in colorectal cancer — cause or consequences? A systematic review, Cancer Cell International, 2021.
- Oral pathobiont induces systemic inflammation and metabolic changes associated with alteration of gut microbiota, Scientific Reports, 2014.
- Periodontal bacteria influence systemic diseases through the gut microbiota, Frontiers in Cellular and Infection Microbiology, 2024.
- Fusobacterium nucleatum and colorectal cancer: From phenomenon to mechanism, Frontiers in Cellular and Infection Microbiology, 2022.
Gateway to Health is the new health & wellness division of The Urban Monk. We've moved the health and life sciences content here and are leaving the personal development and mindfulness materials on theurbanmonk.com.
Disclaimer: This content is for educational purposes only and is not intended to diagnose, treat, cure, or prevent any disease. Please consult a qualified healthcare professional before making changes to your health protocol.







