The Teeth and Bone Health Connection Your Tests Missed
Jan 22, 2026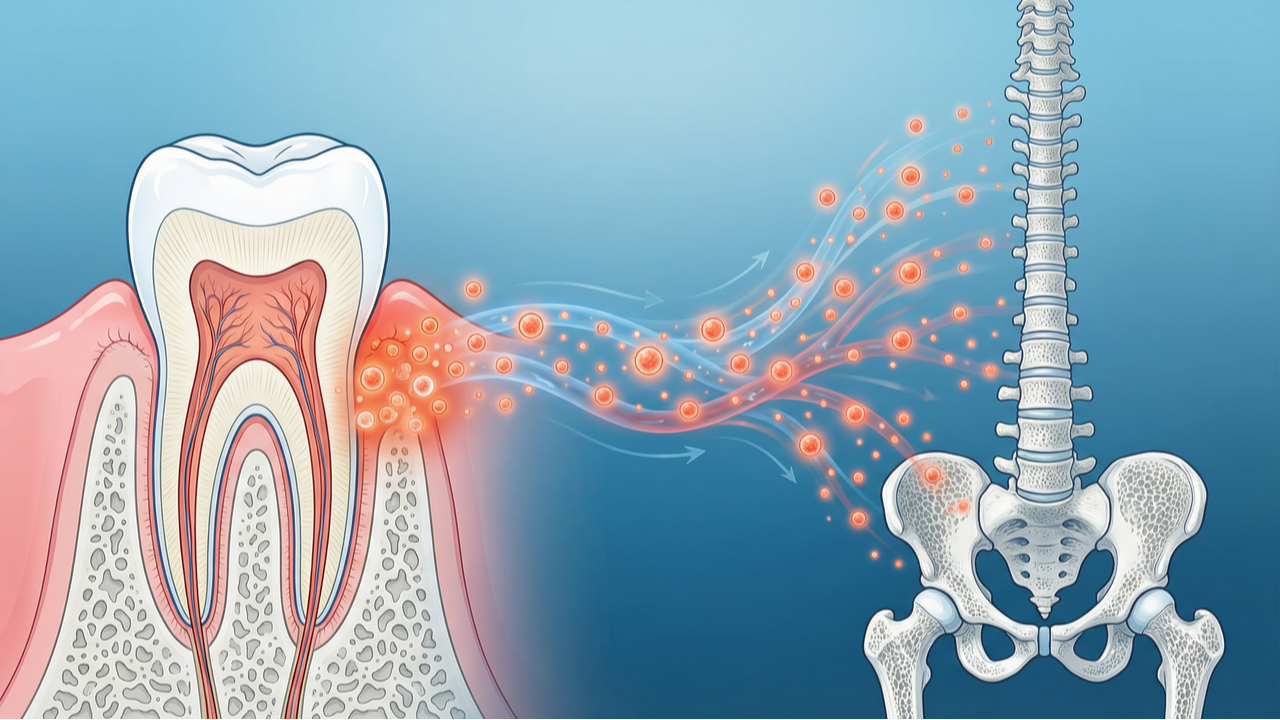
The Teeth and Bone Health Connection Hiding Behind Your Gum Disease
Sarah had been seeing her endocrinologist for declining bone density and her dentist for receding gums — both excellent practitioners treating what they saw in their respective specialties.
But it wasn't until three years and two dental implant failures later that someone finally looked at both conditions together and recognized they might be connected.
The specialists she'd been seeing simply weren't trained to make that connection across disciplines.
If you're experiencing both gum disease and bone loss, you're not alone — and more importantly, these conditions are far more connected than most practitioners realize.
The teeth and bone health connection runs deeper than standard dental and medical appointments typically address, and understanding this relationship might explain why your treatments haven't been working.
Throughout this article, you'll discover how inflammation from your mouth travels throughout your skeletal system, the specific mechanisms driving bone loss in both your jaw and the rest of your body, and why comprehensive oral microbiome testing reveals connections that routine dental exams and bone density scans miss.
You'll also learn about actionable steps you can take right now to address both conditions at their root cause rather than managing symptoms indefinitely.
Discover the Oral-Systemic Connection
Free 10-Day Screening • Gateway to Health Documentary Series
Learn how gum disease drives bone loss throughout your body
Hear from leading dental researchers and functional medicine experts
Understand the inflammatory pathways connecting oral and skeletal health
Key Takeaways
- Periodontal disease and osteoporosis share inflammatory pathways that accelerate bone loss throughout your entire skeletal system — not just your jaw.²,⁵
- Women with osteoporosis show significantly higher rates of clinical attachment loss, deeper periodontal pockets, and more gingival bleeding than those without systemic bone loss.¹
- The same inflammatory cytokines destroying alveolar bone around your teeth are simultaneously breaking down bone density in your hips, spine, and throughout your skeleton.⁴,⁵
- Specific oral pathogens like Porphyromonas gingivalis trigger systemic inflammation that promotes osteoclast activity (bone breakdown) while inhibiting osteoblast function (bone formation).³,⁴
- Vitamin D, K2, calcium, and magnesium deficiencies affect both oral and skeletal health simultaneously.⁷,⁹,¹¹,¹³
- Gut bacteria also influence jawbone health through systemic inflammation.⁶
- Oral microbiome testing identifies specific pathogenic bacteria driving both gum disease and systemic bone loss, allowing for targeted interventions instead of guesswork.
Identify the Pathogens Driving Your Bone Loss
Comprehensive Oral Microbiome Testing + Personalized Health Coaching
Discover which specific bacteria are destroying bone in your mouth and body
Get targeted protocols based on your unique bacterial profile
Work with licensed practitioners who understand oral-systemic connections
When the Oral-Systemic Connection Gets Overlooked
Here's what typically happens in modern healthcare:
You visit your dentist for bleeding gums and receding tissue. They provide expert care within their specialty — diagnosing periodontal disease, recommending a deep cleaning, perhaps prescribing an antimicrobial rinse.
Meanwhile, your physician orders a DEXA scan, confirms low bone density, and suggests evidence-based treatments like calcium supplements or medication.
Each practitioner is delivering excellent care within their scope of practice.
The challenge isn't the quality of care — it's that these specialists often work in separate systems without opportunities to connect the dots between oral and skeletal health.
But recent research reveals something these standard appointments aren't designed to address.
Studies examining 5,736 participants found that people with osteoporosis showed significantly higher rates of clinical attachment loss, deeper probing depths, more gingival recession, and increased bleeding on probing compared to those without systemic bone loss.¹
The connection isn't coincidental — it's mechanistic.
Both periodontitis and osteoporosis are chronic inflammatory diseases characterized by bone resorption.
While osteoporosis involves systemic skeletal deterioration, periodontitis causes localized destruction of the alveolar bone supporting your teeth.²
What ties them together is inflammation's profound impact on bone metabolism throughout your entire skeletal system.
What's emerging from research is that dental and medical specialties have traditionally operated independently — dentistry focusing on oral health, medicine focusing on systemic health.
This specialization has been essential for advancing each field, but it means the oral-systemic connection linking both conditions isn't always part of standard training or practice protocols.
See What Your Specialists Are Missing
Free 10-Day Limited Screening
Why dental and medical care often work in silos, missing critical connections
The mechanistic link between gum disease and osteoporosis explained by experts
How to bridge the gap between dental and medical approaches to bone health
The Inflammatory Cascade Destroying Your Bones
Understanding how oral health and chronic disease are connected requires looking at what happens when oral pathogens trigger systemic inflammation.
When pathogenic bacteria like Porphyromonas gingivalis, Tannerella forsythia, and Fusobacterium nucleatum colonize beneath your gum line, they don't stay confined to your mouth.
These bacteria produce inflammatory mediators that activate your immune system — not just locally, but systemically.³
Here's the mechanism:
Inflammatory cytokines such as tumor necrosis factor (TNF), interleukin-1 (IL-1), and interleukin-6 (IL-6) become elevated in response to oral pathogens. These same cytokines activate specialized cells called osteoclasts, which break down bone tissue.
Simultaneously, this inflammatory environment inhibits osteoblasts — the cells responsible for building new bone.⁴
The result? Net bone loss. Not just in your jaw, but throughout your skeletal system.
How Oral Bacteria Destroy Bone Throughout Your Body
Step 1: Pathogenic Bacteria Colonize
P. gingivalis, T. forsythia, and F. nucleatum establish beneath your gum line
Step 2: Inflammatory Response Triggered
Your immune system releases TNF, IL-1, and IL-6 cytokines systemically
Step 3: Osteoclasts Activated
Cytokines activate bone-breaking cells that begin destroying tissue
Step 4: Osteoblasts Inhibited
Same inflammation blocks bone-building cells from repairing damage
Result: Net Bone Loss
Progressive deterioration in both your jaw and throughout your skeletal system
Research from multiple institutions confirms this connection.
Studies show that inflammation disrupts the balance between bone resorption and bone formation, creating what researchers call "uncoupled" bone remodeling.⁵
Enhanced cytokine production and elevated inflammatory responses exacerbate osteoclastic bone resorption while inhibiting osteoblastic bone formation — a perfect storm for progressive bone loss in both your mouth and the rest of your body.
Understanding the Mechanisms Destroying Your Bones
Free 10-Day Limited Screening • Experts Explain Oral-Systemic Health
Discover how oral health drives systemic inflammation throughout your body
Learn the connections between oral bacteria and chronic diseases
Hear from leading experts on cutting-edge oral health innovations
The Mouth-Gut-Bone Axis Nobody's Talking About
The connection between your teeth and bones extends beyond direct oral inflammation.
Emerging research reveals that gut bacteria also play a critical role in jawbone health⁶ — creating a mouth-gut-bone axis that's only recently being understood in clinical practice.
Scientists at the Medical University of South Carolina discovered that specific gut bacteria trigger immune responses that directly influence alveolar bone metabolism.⁶
When gut microbiome composition shifts toward inflammatory species, these bacteria activate immune cells that travel to distant skeletal sites⁶, including your jawbone, where they promote bone resorption.
This finding challenges the assumption that bone loss in your mouth is regulated solely by oral bacteria.
The reality is more complex: dysbiosis in your gut amplifies the inflammatory environment that oral pathogens exploit, accelerating bone destruction in both local and systemic sites.
The Mouth-Gut-Bone Connection
Three interconnected systems affecting your skeletal health
Oral Microbiome
Pathogenic bacteria colonize beneath gums
Bidirectional Influence
Gut Microbiome
Dysbiosis triggers immune responses
Systemic Effect
Bone Health
Inflammation from both oral and gut bacteria promotes bone breakdown in your jaw and throughout your skeleton
Key Insight: You cannot address bone loss effectively by treating oral or gut health in isolation. The systems are interconnected.
Patients with inflammatory bowel conditions like Crohn's disease — where specific gut bacteria flourish — frequently develop severe periodontal disease and alveolar bone loss.⁶
The connection isn't accidental. It demonstrates that restoring balance to both your oral and gut microbiomes is essential for protecting your skeletal health.
Your Gut May Be Destroying Your Jawbone
Test for Gut Permeability, Inflammation & Bacterial Imbalances
Identify gut bacteria triggering immune responses that attack your bones
Measure intestinal permeability (leaky gut) driving systemic inflammation
Get targeted protocols to restore gut-bone health balance
Why Nutrient Deficiencies Hit Both Systems
Calcium, vitamin D, K2, and magnesium are frequently mentioned as essential for bone health.
What's less commonly discussed is how deficiencies in these nutrients affect both your jawbone and your skeletal system simultaneously — and how oral microbiome dysfunction interferes with nutrient metabolism.
Vitamin D plays a crucial role in calcium absorption and bone mineralization.
Chronic low vitamin D intake leads to negative calcium balance and bone loss in alveolar bone just as it does in other bones throughout your body.⁷
Clinical studies have consistently demonstrated an inverse relationship between serum vitamin D levels and periodontal disease inflammation, with low vitamin D associated with increased severity of periodontitis.⁸
But here's what conventional supplementation misses: vitamin D also reduces inflammation through its anti-inflammatory and antimicrobial properties — one of the key mechanisms linking gum disease to systemic conditions.
Without addressing the inflammatory burden from oral pathogens, simply taking vitamin D supplements provides incomplete protection.
Vitamin K2 presents an even more overlooked connection. This nutrient activates osteocalcin, a protein hormone that binds calcium into your bone matrix — including your jawbone.
Without adequate K2, osteocalcin remains undercarboxylated and cannot effectively promote bone mineralization.⁹
Research confirms that vitamin K2 supplementation significantly improves bone metabolism by enhancing osteocalcin carboxylation while reducing undercarboxylated osteocalcin levels.¹⁰
Interestingly, vitamin K2 is produced by gut bacteria¹¹, which means gut microbiome imbalances can impair your body's ability to generate this critical nutrient naturally.
This creates a vicious cycle: oral and gut dysbiosis drives inflammation that destroys bone, while simultaneously reducing your capacity to produce nutrients essential for bone repair.
The synergistic relationship between vitamins D3 and K2 is particularly important.
D3 helps your body absorb calcium, while K2 directs that calcium to bones and teeth rather than soft tissues.¹¹ Without both working together, supplementation provides limited benefit.
Magnesium also plays a critical role in bone health.
Studies show that higher magnesium intake is associated with increased bone mineral density, with research demonstrating that lower serum magnesium values are related to the presence of osteoporosis.¹³
Approximately 50-60% of the body's magnesium resides in bone tissue, where it serves as a component of the hydroxyapatite mineral structure.¹⁴
What Standard Tests Are Missing
Here's the frustrating reality: your routine dental cleaning and annual DEXA scan aren't designed to identify the underlying drivers of bone loss in either location.
Standard periodontal examinations measure pocket depths and attachment loss but don't identify which specific bacterial species are colonizing beneath your gums.
Similarly, bone density scans reveal that you've lost bone mass but provide no information about why this is happening or how to address the root cause.
This is where oral microbiome testing becomes invaluable. Unlike surface-level assessments, comprehensive testing identifies the specific pathogenic bacteria driving inflammation and bone destruction.
Standard Testing vs. Comprehensive Testing
Standard Testing Limitations
Dental Cleaning: Measures pocket depth only
DEXA Scan: Shows bone loss, not the cause
No bacterial ID: Can't identify specific pathogens
Result: Generic protocols & incomplete picture
Comprehensive Testing Approach
Oral Microbiome Test: DNA sequencing identifies exact bacterial species
Gut Testing: Reveals inflammatory markers & permeability
Root cause ID: Pinpoints specific pathogens driving bone loss
Result: Targeted interventions & complete health picture
Tests like the Orobiome panel analyze bacterial populations that standard dental exams overlook entirely, revealing hidden connections between your oral health and systemic conditions.
When you understand which oral pathogens are present and at what levels, you can implement targeted interventions rather than generic protocols that may or may not address your specific situation.
The testing package includes personalized oral health coaching that guides you toward the right nutrients, probiotics, and antimicrobial strategies specific to your bacterial profile — not one-size-fits-all recommendations.
For those wondering whether gut bacteria might be contributing to oral bone loss, specialized gut testing that measures intestinal permeability markers like zonulin, lipopolysaccharide (LPS) antibodies, and specific food sensitivities provides the missing piece of the puzzle.
Stop Guessing. Start Testing.
Identify Specific Bacteria • Personalized Protocol • Expert Coaching
DNA sequencing reveals exact bacterial populations destroying your bone health
Licensed oral health professionals interpret your results and create custom protocols
Targeted solutions instead of one-size-fits-all dental advice
Breaking the Cycle of Bone Loss
Understanding the teeth and bone health connection is one thing. Addressing it effectively often requires an integrative approach that brings together insights from multiple specialties.
First, recognize that treating gum disease and osteoporosis as separate conditions will continue yielding incomplete results.
The inflammatory pathways are shared, the nutrient deficiencies affect both systems, and the microbial imbalances drive destruction in multiple locations simultaneously.
Research confirms that people with low systemic bone mineral density face greater risk for developing severe periodontitis and tooth loss, while those with advanced periodontal disease show accelerated systemic bone loss.¹²
This bidirectional relationship means that addressing one without the other leaves you vulnerable to continued deterioration.
Second, move beyond symptom management toward root cause resolution.
Calcium supplements won't reverse bone loss if inflammatory cytokines continue promoting osteoclast activity.
Deep cleanings won't prevent bone destruction if pathogenic oral bacteria immediately recolonize.
Medications that slow bone resorption don't address why your body lost the ability to maintain bone homeostasis in the first place.
The solution requires restoring balance to your oral microbiome, addressing systemic inflammation, correcting nutrient deficiencies with properly balanced supplementation, and supporting both gut and oral health simultaneously.
Third, work with practitioners who understand these connections.
Many dentists and physicians are now receiving training in oral-systemic health and can coordinate care effectively.
Dentists with this training can partner with medical providers to create comprehensive treatment plans, while functional medicine practitioners can incorporate oral microbiome assessment to provide a complete picture of your health.
Your Next Steps
If you're experiencing both gum disease and bone loss — or if you've been diagnosed with one and want to prevent the other — here's what to consider:
Start by assessing your oral microbiome.
Oral microbiome testing reveals which specific bacterial populations are driving inflammation and bone destruction, allowing for targeted interventions.
The comprehensive package includes personalized coaching to help you interpret results and implement effective protocols.
If you suspect gut health might be contributing to your oral bone loss, consider comprehensive gut testing that examines inflammatory markers, intestinal permeability, and bacterial populations affecting systemic inflammation.
Watch the Gateway to Health documentary series for free during the 10-day screening period.
You'll learn from leading dental researchers and clinicians about emerging connections between oral health and chronic diseases.
Focus on gum disease prevention through oral microbiome balance rather than sterility.
Your mouth needs healthy bacterial populations to resist pathogenic colonization — an approach fundamentally different from antimicrobial rinses that indiscriminately eliminate all bacteria.
Remember that bleeding gums aren't just a dental issue.
They signal inflammation that may be affecting your brain, heart, and skeletal health simultaneously. Addressing them comprehensively rather than superficially protects far more than just your teeth.
The teeth and bone health connection represents an evolving understanding in healthcare.
When you address the shared inflammatory pathways, microbial imbalances, and nutrient deficiencies driving both periodontal disease and osteoporosis alongside your regular dental and medical care, you create the conditions for comprehensive healing and long-term health.
Your mouth has been trying to tell you something about your skeletal health. It's time to listen.
Take the First Step to Protecting Your Bones
Oral Microbiome Testing Reveals Hidden Drivers of Bone Loss
Comprehensive bacterial DNA analysis identifies pathogens attacking your bones
One-on-one consultation with Dr. Elmira Shojai's team of licensed oral health professionals
Personalized healing protocol targeting your specific oral-systemic challenges
Sources
- Association between periodontitis and osteoporosis in United States adults from the National Health and Nutrition Examination Survey: a cross-sectional analysis. BMC Oral Health. 2023.
- Osteoporosis and periodontal diseases – An update on their association and mechanistic links. Periodontology 2000. 2022.
- Mechanism of alveolar bone destruction in periodontitis — Periodontal bacteria and inflammation. Japanese Dental Science Review. 2021.
- Inflammation and Uncoupling as Mechanisms of Periodontal Bone Loss. Journal of Dental Research. 2011.
- Osteoporosis and Periodontitis. Curr Osteoporos Rep. 2017.
- The Gut's Role in Oral Bone Health. National Institute of Dental and Craniofacial Research. 2022.
- One-year Effects of Vitamin D and Calcium Supplementation on Chronic Periodontitis. Journal of Periodontology. 2012.
- The role of vitamin D in periodontal health and disease. Journal of Periodontal Research. 2023.
- Role of vitamin K2 in bone metabolism: a point of view and a short reappraisal of the literature. Gynecological Endocrinology. 2020.
- The effect of vitamin K2 supplementation on bone turnover biochemical markers in postmenopausal osteoporosis patients: a systematic review and meta-analysis. Frontiers in Endocrinology. 2025.
- The combined effect of vitamin K and calcium on bone mineral density in humans: a meta-analysis of randomized controlled trials. Journal of Orthopaedic Surgery and Research. 2021.
- Association between periodontitis and osteoporosis in United States adults from the National Health and Nutrition Examination Survey. BMC Oral Health. 2023.
- An update on magnesium and bone health. BioMetals. 2021.
- The role of magnesium in the pathogenesis of osteoporosis. Frontiers in Endocrinology. 2024.
Gateway to Health is the new health & wellness division of The Urban Monk. We've moved the health and life sciences content here and are leaving the personal development and mindfulness materials on theurbanmonk.com.
Disclaimer: This content is for educational purposes only and is not intended to diagnose, treat, cure, or prevent any disease. Please consult a qualified healthcare professional before making changes to your health protocol.







